CellR4 2014; 2 (2): e883
Possible consequences of non-adherence to immunosuppression: a case of acute T-Cell mediated kidney rejection and IgA nephropathy
Topic: Stem cells
Category: Case Reports
Abstract
T-cell dysregulation plays an important role in IgAN pathogenesis and recurrence post kidney transplantation.
We describe the case of a 52 years old Asian woman with IgAN who received an unrelated living donor kidney transplant. She had independently withdrawn all immunosuppressive maintenance therapy seven years after transplantation followed by acute kidney dysfunction. Acute T-cell mediated rejection was demonstrated in the first kidney biopsy. High steroid pulses were administered with partial response. Recurrence of native IgAN associated with partial resolution of T-cell mediated rejection was observed, as showed in the second kidney biopsy.
We hypothesize that recurrence of primary nephropathy could be a manifestation of T-cells activation in non-adherent patients partially responsive to T-cell anti-rejection therapy.
INTRODUCTION
Immunoglobulin A nephropathy (IgAN) is a frequent cause of glomerulonephritis more common in Asia than the rest of the world 1 , 2. IgAN is characterized by polymeric IgA deposition and accumulation in the glomerular mesangium 3. Although IgAN is considered a benign disease, it causes chronic renal failure in 20-40% of patients 4 , 5. Patients with primary IgAN usually represent ideal candidates for renal transplantation because they are often relatively young with little comorbidity 6 , 7.
Recurrence of primary glomerular nephropathy after renal transplant occurs in 10-20% of kidney grafts and accounts for graft failure in up to 50% of cases. IgA nephropathy represents the most frequent form of recurrent glomerulonephritis with histological evidence of IgAN recurrence in up to 60% of chronic kidney dysfunction, occurring usually within the first 3-4 years after transplantation 8 , 9 , 10. However, factors predicting the recurrence of IgAN remain controversial. Several studies have reported a higher risk of disease recurrence among organs from living-related donors 11 , 12. Therefore, in native IgAN, improvement in increasing of steroid treatment is required after kidney transplantation.
T-cell dysregulation plays an important role in IgAN pathogenesis and recurrence. T-cells are involved in IgA production, which accumulate in glomerular mesangium 13. In patients with severe manifestation, immunosuppressive therapy with cyclophosphamide, azathioprine or mycophenolate mofetil (MMF) is usually recommended 14, 15 , 16. Their therapeutic effects seem to be related to the ability to regulate T-cell immunity and the Th1/Th2 balance 17.
Compliance to immunosuppressive treatment is necessary to prevent rejection and graft loss in solid organ transplantation. Non-adherence to immunosuppressive regimen has been shown in 20 to 37% of kidney transplant recipients 18 , 19 , 20 , 21.
Systematic reviews have shown that an estimated 50% (range 20-73%) of late acute rejections and 15% (range 3-35%) of graft losses are associated with non-adherence to the therapeutic regimen 22 , 23 , 24. Non-adherence to immunosuppressant therapy is one of the major causes of early and late renal acute rejection and allograft failure. Even if association between recurrent IgAN and acute rejection has not been found 25, we hypothesize that recurrence of primary nephropathy could be a manifestation of T-cells activation in non-adherent patients or in partial responsive T-cell rejection patients.
CASE REPORT
Here we describe a case of a 52 years old Asian woman with an history of end stage renal disease on haemodialysis secondary to IgAN since 2004 who received an unrelated living donor kidney transplant (LDKT) in the Philippines on October 2006 (negative T-cell cross match), as evidenced by patient’s medical record from Hospital of Philippine (Ortigas Center, Pasig City). Her immunosuppressive therapy was based on MMF, steroids and calcineurin inhibitors (cyclosporine then replaced with tacrolimus in December 2006).
The patient came to our outpatient nephrology clinic in January 2007. Follow-up visit were scheduled weekly over the first month and every 4-6 weeks thereafter, until 12 months after transplant. Thereafter, follow-up visits were scheduled every 3-4 months. Immunosuppressive drug trough levels, routine bloods and urinalysis were monitored each time. Blood tests and imaging showed satisfactory function of the transplanted kidney with serum creatinine (sCre) levels ranging from 0.5 to 0.7 mg/dL till October 2011. Since then, the patient failed to attend the scheduled appointments and omitted to check immunosuppression level. She returned to our attention on March 3, 2013 when she was admitted to the Emergency Department at the Policlinico Umberto I in Rome for anuria and general maculopapular rash. Laboratory investigation at admission in Nephrology Department and Transplant Unit (March 5, 2013), revealed worsening of renal function, with extremely high sCre levels (20 mg/dL), blood urea nitrogen (BUN) of 148 mg/dL, severe metabolic acidosis, hyponatremia and hyperphosphoremia (Table 1). The chest x-ray showed multiple nodular thickening partially confluent in the right lung and bilaterally emphasizing of bronco-vascular structures.
Medical treatment was commenced to correct metabolic acidosis in association with intravenous antibiotic therapy and renal replacement therapy was started after insertion of central femoral line. Blood tests and clinical conditions improved during the following days with resolution of chest x-ray multiple nodularity and of maculopapular rash. Hemolytic uremic syndrome diagnosis was excluded because of normal platelets count (327.000 cells/mm3) and absence of hemolytic signs or schistocytes in peripheral blood. Negative test for ANA, c/pANCA, ENA, C3, C4, ACA, LAC, and normal IgG/A/M dosage excluded the occurrence of autoimmune glomerulonephritis. Further anamnestic investigations revealed that the patient had independently withdrawn all immunosuppressive maintenance therapy over the last 3 months.
The ultrasound scan with Doppler sonography (March 6, 2013) showed: increased size (maximum longitudinal diameter of 143.3 mm) and regular shape of the transplanted kidney; reduction of cortico-medullary differentiation with hyperechoic cortex; no urinary tract dilatations; patent renal vein with normal flow in the absence of wall alterations; iliac-renal anastomosis and renal artery were patent; resistive index 0.70. Donor specific anti-HLA antibodies were not assessed because the transplant was performed from a living donor abroad. In the suspicion of acute allograft rejection, a first renal biopsy was performed (March 7, 2013). It showed the presence of acute T-cell mediated rejection (t3, i3, v1, g0) 26 with mild-moderate intimal arteritis and absence of IgA deposits (negative immunofluorescence – IF). C4d staining was negative (Figure 1).
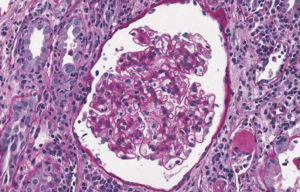
Figure 1. First histopathological renal examination by Periodic Acid Schiff reaction, x25. Light microscopy shows inflammatory infiltration of mononuclear cells associated with quite mild increase in mesangial matrix. Detachment of the epithelium of tubules due to marked inflammatory infiltration with tubulitis. Occasional necrosis and denudation of basement membranes with significant reactive nuclear atypia. Arteries show inflammatory infiltration of mononuclear cells. In the arteries intimal thickening is present with reduction of lumen. There is accompanying focal interstitial edema and interstitial fibrosis.
After exclusion of on-going infectious process (PCR analysis for HSV, CMV, EBV, VZV, BKV resulted negative) a first high dose steroid pulse (methylprednisolone 1 g/day for 3 days and decalage) was administered followed by resumption of diuresis and reduction of transplanted kidney size (maximum longitudinal diameter of 133.3 mm). At the same time, immunosuppressive therapy was reintroduced and increased, maintaining tacrolimus and MMF levels into the higher side of therapeutic range. On March 13 the patient underwent to a second high dose steroid bolus/pulse (methylprednisolone 500 mg/day for 3 days and decalage) with further improvement in overall clinical condition and blood tests (sCre 5.3 mg/dL, BUN 61 mg/dL, serum sodium 130 mmol/L, serum potassium 4.56 mmol/L), proteinuria 605 mg/24h, therefore hemodialysis was stopped. On April 8 renal ultrasonography showed further reduction of transplanted kidney size compared to the previous control (maximum longitudinal diameter of 120.0 mm). Despite this initial clinical improvement a worsening of sCre value and needing of restarting renal replacement therapy occurred. A third high dose steroid pulse (methylprednisolone 500 mg/day for 3 days and decalage) was administered without benefits and a second kidney biopsy (April 10, 2013) was performed within one month after the previous one. This yielded partial resolution of T-cell mediated rejection features (t1, i1, v0, g0) associated with significant interstitial fibrosis. Immunofluorescence, which was negative in the previous biopsy, showed an unexpected high positivity with a diffuse mesangial granular IgA deposits onset with the features of diffuse proliferative IgAN. C4d staining was occasionally positive in peritubular capillaries in the context of the major areas of fibrosis (Figure 2).

Figure 2. Second histopathological renal examination by immunofluorescence. Immunofluorescence shows fairly diffuse, predominantly granular mesangial staining for IgA (+++), IgM (+++), C3 (++), kappa (+) and lambda (++) light chains. No staining for IgG, C1q and fibrinogen.
The persistence, even if improved, of cell mediated rejection associated to the appearance of IgA tissue deposits would have required additional therapies such as immunoglobulins, plasmapheresis and/or biologic drugs but the presence of significant and diffuse interstitial fibrosis and the appearance of labial Herpetic lesion discouraged these additional and expensive interventions. Therefore, we suggested commencing chronic renal replacement therapy after creation of an arteriovenous fistula.
DISCUSSION
The availability of new immunosuppressive protocols has allowed a significant improvement in the survival of transplanted kidney. Acute rejection by non-adherence to immunosuppressive therapy may occur at any time after transplantation, and can be either cellular-mediated (named T-cell involvement) or humoral (B-cell involvement). Our clinical case suggests that non-adherence to immunosuppressive therapy has not only determined T-mediated rejection, but also the emergence of a primary IgAN, which is recognized to be characterized by a T-cell deregulation 27 , 28 , 29.
In previous studies, increases in IgA-containing B lymphocytes, IgA-specific T-helper cells, and decreased activity of IgA-specific suppressor T-cells were observed in IgAN patients 30 , 31 , 32. These results implicate lymphocyte dysregulation in IgAN suggesting an important role for T lymphocytes in the development of IgAN.
In our patients in fact, non clinical or biochemical signs of glomerulonephritis were observed after transplantation, neither IgA mesangial deposits resulted on the first kidney biopsy performed seven years after transplantation. Diffuse IgA deposition appeared only on the second kidney biopsy associated to creatinine elevation, presumably as complication of incomplete response to anti-rejection therapy resulting from T-cells activation. Partial T-cell response associated to the presence of risk factor for IgAN, as suggested by the native IgAN, and non-adherence to immunosuppression, may have facilitated IgAN recurrence after T-cell rejection. The development of complications such as diffuse interstitial fibrosis and Herpetic infection discouraged additional immunosuppressive interventions.
Mesenchymal stem cells (MSCs) have been studied in the context of nephrology 33. These cells can differentiate into various cell types, migrate to sites of tissue injury, and enhance repair by secreting antifibrotic and proangiogenic factors 34 , 35 , 36. Mesenchymal stem cells treatment showed no evidence of adverse events such as procedure-related events, acute toxicity, organ system complications, infection, death, or malignancy.
Results of recent clinical trials supported safety and promising effects of autologous and allogeneic MSCs in solid organ transplantation reducing ischemia-reperfusion injury and promoting immune tolerance. In particular, in patients undergoing living-related donor kidney transplants the use of MSCs was compared with anti-IL-2 receptor antibody induction therapy and standard-dose of calcineurin inhibitors showing reduced risk of opportunistic infection, lower incidence of rejection, ability to omit induction and/or lower maintenance immunosuppression regimen, with better estimated renal function at 1 year 37 , 38 , 39.
Over the past few years, adipose tissue has attracted much research attention because adipose-derived stem cells (ASCs) contain greater numbers of MSCs than bone marrow-derived stem cells from bone marrow 40. Adipose-derived stem cells can be more easily collected and isolated, are relatively more abundant, can be expanded and proliferate more rapidly and carry a lower harvesting risk than bone marrow stem cells. Adipose-derived stem cells have been reported to be able to prevent tissue damage through immune-modulating effects in mouse model.
Hyun et al 41 examined the potential therapeutic effects of ASCs treatment in IgAN showing Th1 predominance in IgAN. This was an important demonstration that ASCs treatment can be used to treat IgAN by modulating the Th1/Th2 cytokine balance through paracrine mechanisms. Interestingly, a case report described disappearance of IgA deposition in a patient diagnosed with IgAN, after peripheral blood stem cell transplantation for acute lymphocytic leukemia 42. These studies suggest that ASCs are valuable therapeutic option for the management of IgAN.
Moreover, peripheral blood stem cells differentiate in renal resident cells and contribute to the improvement of glomerular injury 43 , 44. In light of these considerations, bone marrow transplantation could be an advantageous therapeutic approach for the treatment of glomerulonephritis also in humans. Some authors speculated on the possibility that Peripheral Blood Stem Cell from a healthy donor could replace injured renal resident cells and contribute to remodeling of injured glomeruli.
Bone marrow transplantation has showed evidence to attenuate kidney diseases including lupus nephritis 45 and IgAN 46 in experimental models. Their therapeutic effect is related to their ability to regulate T-cell immunity and the Th1/Th2 balance. In fact, ASCs therapy significantly decreased Th1 cytokine activity in the kidney and caused a shift to Th2 responses in spleen T-cells as determined by fluorescence-activated cell sorter analysis 47. Only recently it has been postulated the application of peripheral blood stem cells. However, this technology could be extended to administer other cell-based therapies.
CONCLUSIONS
With our case we want to describe the effects of non-adherence to immunosuppressive therapy after kidney transplantation on T-cells activation causing the onset of cellular rejection and IgAN in a patient with history of IgAN.
Non-adherence to immunosuppressive therapy is the major cause of rejection and in this case it could also have led to recurrence of primary nephropathy resulting in a synergic negative impact on the transplant outcome. The poor response to therapy promptly performed did not modify the IgAN recurrence and the related poor graft outcome.
In our case, the use of stem cells might have a role both on T-cell mediated rejection and on IgAN recurrence, which is known to be linked to T-cells dysregulation.
We suggest the use of stem cells as possible therapeutic choice to improve the renal outcome in T-cells dysfunction in kidney transplant complications.
ACKNOWLEDGEMENTS
We thank Prof. Andrea Onetti Muda (Department of Human Anatomy, Campus Bio-Medico of Rome; Rome, Italy) who performed histopathological examination of renal biopsies.
Conflict of Interests: The Authors declare that they have no conflict of interests.
REFERENCES
- D’Amico G. The commonest glomerulonephritis in the world: IgA nephropathy. Q J Med 1987; 64: 709-727. (back)
- Woo KT, Chan CM, Chin YM, Choong HL, Tan HK, Foo M, Anantharaman V, Lee GS, Chiang GS, Tan PH, Lim CH, Tan CC, Lee E, Tan HB, Fook-Chong S, Lau YK, Wong KS. Global evolutionary trend of the prevalence of primary glomerulonephritis over the past three decades. Nephron Clin Pract 2010; 116: c337-c346. (back)
- Galla JH. IgA nephropathy. Kidney Int 1995; 47(2): 377-387. (back)
- Asaba K, Tojo A, Onozato ML, Kinugasa S, Miyazaki H, Miyashita K, Uehara Y, Hirata Y, Kimura K, Goto A, Omata M, Fujita T. Long-term renal prognosis of IgA nephropathy with therapeutic trend shifts. Intern Med 2009; 48: 883-890. (back)
- Imai H, Nakamoto Y, Asakura K, Miki K, Yasuda T, Miura AB. Spontaneous glomerular IgA deposition in ddY mice: An animal model of IgA nephritis. Kidney Int 1985; 27: 756-761. (back)
- Odum J, Peh CA, Clarkson AR, Bannister KM, Seymour AE, Gillis D, Thomas AC, Mathew TH, Woodroffe AJ. Recurrent mesangial IgA nephritis following renal transplantation. Nephrol Dial Transplant 1994; 9: 309-312. (back)
- Ortiz F, Gelpi R, Koskinen P, Manonelles A, Räisänen-Sokolowski A, Carrera M, Honkanen E, Grinyó JM, Cruzado JM. IgA nephropathy recurs early in the graft when assessed by protocol biopsy. Nephrol Dial Transplant 2012; 27: 2553-2558. (back)
- Odum J, Peh CA, Clarkson AR, Bannister KM, Seymour AE, Gillis D, Thomas AC, Mathew TH, Woodroffe AJ. Recurrent mesangial IgA nephritis following renal transplantation. Nephrol Dial Transplant 1994; 9: 309-312. (back)
- Ortiz F, Gelpi R, Koskinen P, Manonelles A, Räisänen-Sokolowski A, Carrera M, Honkanen E, Grinyó JM, Cruzado JM. IgA nephropathy recurs early in the graft when assessed by protocol biopsy. Nephrol Dial Transplant 2012; 27: 2553-2558. (back)
- 8 (back)
- Namba Y, Oka K, Moriyama T, Ichimaru N, Kyo M, Kokado Y, Ito T, Imai E, Aozasa K, Okuyama A, Takahara S. Risk factors for graft loss in patients with recurrent IGA nephropathy after renal transplantation. Transplant Proc 2004; 36(5): 1314-1316. (back)
- Freese P, Svalander C, Norden G, Nyberg G. Clinical risk factors for recurrence of IgA nephropathy. Clin Transplant 1999; 13: 313-317. (back)
- Galla JH. IgA nephropathy. Kidney Int 1995; 47(2): 377-387. (back)
- Pozzi C. Andrulli S, Pani A, Scaini P, Del Vecchio L, Fogazzi G, Vogt B, De Cristofaro V, Allegri L, Cirami L, Procaccini AD, Locatelli F. Addition of azathioprine to corticosteroids does not benefit patients with IgA nephropathy. J Am Soc Nephrol 2010; 21: 1783-1790. (back)
- Frisch G, Lin J, Rosenstock J, Markowitz G, D’Agati V, Radhakrishnan J, Preddie D, Crew J, Valeri A, Appel G. Mycophenolate mofetil (MMF) vs placebo in patients with moderately advanced IgA nephropathy: a double-blind randomized controlled trial. Nephrol Dial Transplant 2005; 20: 2139-2145. (back)
- Maes, BD, Oyen R, Claes K, Evenepoel P, Kuypers D, Vanwalleghem J, Van Damme B, Vanrenterghem YF. Mycophenolate mofetil in IgA nephropathy: results of a 3-year prospective placebo-controlled randomized study. Kidney Int 2004; 65: 1842-1849. (back)
- Hyun YY, Kim IO, Kim MH, Nam DH, Lee MH, Kim JE, Song HK, Cha JJ, Kang YS, Lee JE, Kim HW, Han JY, Cha DR. Adipose-Derived Stem Cells Improve Renal Function in a Mouse Model of IgA Nephropathy. Cell Transplantation 2012; 21: 2425-2439. (back)
- De Geest S, Dobbels F, Fluri C, Paris W, Troosters T. Adherence to the therapeutic regimen in heart, lung, and heart-lung transplant recipients. J Cardiovasc Nurs 2005; 20: S88-S98. (back)
- Denhaerynck K, Dobbels F, Cleemput I, Desmyttere A, Schäfer-Keller P, Schaub S, De Geest S. Prevalence, consequences, and determinants of non adherence in adult renal transplant patients: a literature review. Transpl Int 2005; 18: 1121-1133. (back)
- Denhaerynck K, Desmyttere A, Dobbels F, Moons P, Young J, Siegal B, Greenstein S, Steiger J, Vanrenterghem Y, Squifflet JP, van Hooff JP, DeGeest S. Nonadherence with immunosuppressive drugs: U.S. compared with European kidney transplant recipients. Prog Transplant 2006; 16: 206-214. (back)
- Dew MA, Di Martini AF, De Vito Dabbs A, Myaskovsky L, Steel J, Unruh M, Switzer GE, Zomak R, Kormos RL, Greenhouse JB. Rates and risk factors for non adherence to the medical regimen after adult solid organ transplantation. Transplantation 2007; 83: 858-873. (back)
- De Geest S, Dobbels F, Fluri C, Paris W, Troosters T. Adherence to the therapeutic regimen in heart, lung, and heart-lung transplant recipients. J Cardiovasc Nurs 2005; 20: S88-S98. (back)
- Denhaerynck K, Dobbels F, Cleemput I, Desmyttere A, Schäfer-Keller P, Schaub S, De Geest S. Prevalence, consequences, and determinants of non adherence in adult renal transplant patients: a literature review. Transpl Int 2005; 18: 1121-1133. (back)
- Dobbels F, Damme-Lombaert R, Vanhaecke J, De Geest S. Growing pains: non-adherence with the immunosuppressive regimen in adolescent transplant recipients. Pediatr Transplant 2005; 9: 381-390. (back)
- Namba Y, Oka K, Moriyama T, Ichimaru N, Kyo M, Kokado Y, Ito T, Imai E, Aozasa K, Okuyama A, Takahara S. Risk factors for graft loss in patients with recurrent IGA nephropathy after renal transplantation. Transplant Proc 2004; 36(5): 1314-1316. (back)
- Solez K, Colvin RB, Racusen LC, Haas M, Sis B, Mengel M, Halloran PF, Baldwin W, Banfi G, Collins AB, Cosio F, David DS, Drachenberg C, Einecke G, Fogo AB, Gibson IW, Glotz D, Iskandar SS, Kraus E, Lerut E, Mannon RB, Mihatsch M, Nankivell BJ, Nickeleit V, Papadimitriou JC, Randhawa P, Regele H, Renaudin K, Roberts I, Seron D, Smith RN, Valente M. Banff 07 classification of renal allograft pathology: updates and future directions.Am J Transplant 2008; 8(4): 753-760. (back)
- Harper SJ, Allen AC, Pringle JH, Feehally J. Increased dimeric IgA producing B-cells in the bone marrow in IgA nephropathy determined by in situ hybridization for J chain mRNA. J Clin Pathol 1996; 49: 38-42. (back)
- Sakai H, Endoh M, Tomino Y, Nomoto Y. Increase of IgA specific helper T alpha cells in patients with IgA nephropathy. Clin Exp Immunol 1982; 50: 77-82. (back)
- Sakai H, Nomoto Y, Arimori S. Decrease of IgA-specific suppressor T-cell activity in patients with IgA nephropathy. Clin Exp Immunol 1979; 38: 243-248. (back)
- Harper SJ, Allen AC, Pringle JH, Feehally J. Increased dimeric IgA producing B-cells in the bone marrow in IgA nephropathy determined by in situ hybridization for J chain mRNA. J Clin Pathol 1996; 49: 38-42. (back)
- Sakai H, Endoh M, Tomino Y, Nomoto Y. Increase of IgA specific helper T alpha cells in patients with IgA nephropathy. Clin Exp Immunol 1982; 50: 77-82. (back)
- Sakai H, Nomoto Y, Arimori S. Decrease of IgA-specific suppressor T-cell activity in patients with IgA nephropathy. Clin Exp Immunol 1979; 38: 243-248. (back)
- Reinders ME, Fibbe WE, Rabelink TJ. Multipotent mesenchymal stromal cell therapy in renal disease and kidney transplantation. Nephrol Dial Transplant 2010; 25: 17-24. (back)
- Reinders ME, Fibbe WE, Rabelink TJ. Multipotent mesenchymal stromal cell therapy in renal disease and kidney transplantation. Nephrol Dial Transplant 2010; 25: 17-24. (back)
- Okada H, Konishi K, Nakazato Y, Kanno Y, Suzuki H, Sakaguchi H, Saruta T. Interleukin-4 expression in mesangial proliferative glomerulonephritis. Am J Kidney Dis 1994; 23: 242-246. (back)
- Sonoda E, Hitoshi Y, Yamaguchi N, Ishii T, Tominaga A, Araki S, Takatsu K. Differential Regulation of IgA production by TGF-b and IL-5: TGF-beta Induces surface IgA-positive cells bearing Il-5 receptor, whereas IL-5promotes their survival and maturation into IgA-secreting cells. Cell Immunol 1992; 140: 158-172. (back)
- Lalu MM, McIntyre L, Pugliese C, Fergusson D, Winston BW, Marshall JC, Granton J, Stewart DJ. Canadian Critical Care Trials Group. Safety of cell therapy with mesenchymal stromal cells (SafeCell): a systematic review and meta-analysis of clinical trials. PLoS One 2012; 7: e47559. (back)
- Tan J, Wu W, Xu X, Liao L, Zheng F, Messinger S, Sun X, Chen J, Yang S, Cai J, Gao X, Pileggi A, Ricordi C. Induction therapy with autologous mesenchymal stem cells in living-related kidney transplants: a randomized controlled trial. JAMA 2012; 307(11): 1169-1177. (back)
- Pileggi A, Xu X, Tan J, Ricordi C. Mesenchymal stromal (stem) cells to improve solid organ transplant outcome: lessons from the initial clinical trials. Curr Opin Organ Transplant 2013; 18(6): 672-681. (back)
- Bailey AM, Kapur S, Katz AJ. Characterization of adipose-derived stem cells: An update. Curr Stem Cell Res Ther 2010; 5: 95-102. (back)
- Hyun YY, Kim IO, Kim MH, Nam DH, Lee MH, Kim JE, Song HK, Cha JJ, Kang YS, Lee JE, Kim HW, Han JY, Cha DR. Adipose-Derived Stem Cells Improve Renal Function in a Mouse Model of IgA Nephropathy. Cell Transplantation 2012; 21: 2425-2439. (back)
- Iwata Y, Wada T, Uchiyama A, Miwa A, Nakaya I, Tohyama T, Yamada Y, Kurokawa T, Yoshida T, Ohta S, Yokoyama H, IidaH. Remission of IgA Nephropathy after Allogeneic Peripheral Blood Stem Cell Transplantation Followed by Immunosuppression for Acute Lymphocytic Leukemia. Intern Med 2006; 45(22): 1291-1295. (back)
- Ito T, Suzuki A, Imai E, Okabe M, Hori M. Bone marrow is a reservoir of repopulating mesangial cells during glomerular remodeling. J Am Soc Nephrol 2001; 12: 2625-2635. (back)
- Rookmaaker MB, Smits AM, Tolboom H, Van ‘t Wout K, Martens AC, Goldschmeding R, Joles JA, Van Zonneveld AJ, Gröne HJ, Rabelink TJ, Verhaar MC. Bone-marrow derived cells contribute to glomerular endothelial repair in experimental glomerulonephritis. Am J Pathol 2003; 163: 553-562. (back)
- Takeuchi K, Inaba M, Miyashima S, Ogawa R, Ikehara S. A new strategy for treatment of autoimmune diseases in chimeric resistant MRL/lpr mice. Blood 1998; 91: 4616-4623. (back)
- Imasawa T, Nagasawa R, Utsunomiya Y, Kawamura T, Zhong Y, Makita N, Muso E, Miyawaki S, Maruyama N, Hosoya T, Sakai O, OhnoT. Bone marrow transplantation attenuates murine IgA nephropathy: role of a stem cell disorder. Kidney Int 1999; 56: 1809-1817. (back)
- Hyun YY, Kim IO, Kim MH, Nam DH, Lee MH, Kim JE, Song HK, Cha JJ, Kang YS, Lee JE, Kim HW, Han JY, Cha DR. Adipose-Derived Stem Cells Improve Renal Function in a Mouse Model of IgA Nephropathy. Cell Transplantation 2012; 21: 2425-2439. (back)
To cite this article
Possible consequences of non-adherence to immunosuppression: a case of acute T-Cell mediated kidney rejection and IgA nephropathy
CellR4 2014; 2 (2): e883
Publication History
Published online: 01 Apr 2014

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.
